
Create Highly Profitable
Healthcare Systems
Through Physician-
Led Cost Control
Proven Strategies for Lower Costs, Better
Care, and Stronger Physician Partnerships
with Clinically Integrated Network Consulting.
Physician-Led Networks That Drive Immediate Savings
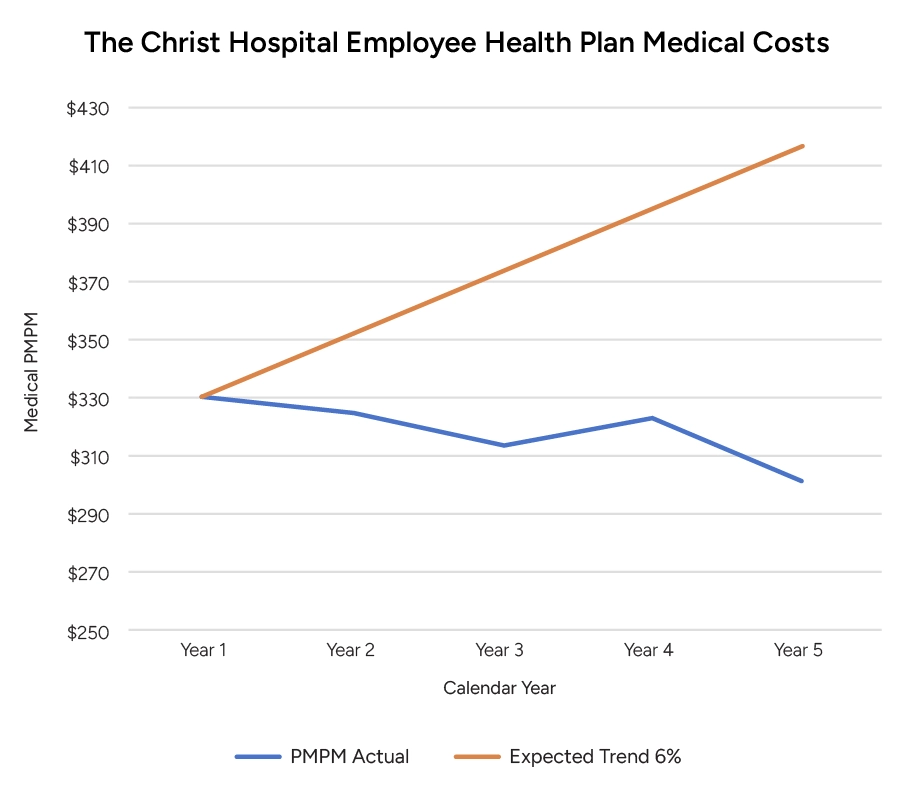
We help hospitals escape fee-for-service traps with physician networks that deliver immediate cost savings.
Our proof? We turned one hospital’s employee health plan into a $60M success story – all while improving patient care and keeping doctors satisfied.
Any of these sound like you?

Struggling with expensive overhead costs?
Staff, supplies, and compliance draining your margins?

Can’t keep raising prices to stay profitable?
The traditional business model just isn’t sustainable anymore.

Worried about switching to value-based care?
Trying to figure out how to make the transition without losing money?

Here’s What Actually Works
We’ve built a physician-led model that transformed employee health spending at Christ Hospital — taking a $42M annual spend in 2012 and generating over $60M in cumulative savings while improving care quality. For systems with larger employee health plans, the savings potential scales proportionally. For example, a system with a $200M annual health spend today could potentially see over $100M in savings, which would be proportionally half of what we achieved at Christ Hospital. This proven approach can stabilize margins and strengthen physician relationships.
Why do Healthcare Systems Struggle to Stay Profitable?
Healthcare systems across America face a critical turning point.
Operating margins continue to shrink while pressure mounts to transition to value-based care models. Hospital CEOs and executives find themselves caught between maintaining current operations and preparing for an uncertain future.
Yet some health systems are thriving in this environment. They’ve discovered how to improve margins while simultaneously preparing for value-based care — without disrupting existing operations or alienating their physician partners.
Their secret lies in a strategically implemented Clinically Integrated Network (CIN) that aligns physician incentives with system goals. It delivers immediate financial returns while building long-term value-based capabilities.
The Redington Difference
With Dr. TJ Redington’s leadership, we’ve generated over $60 million in documented savings and annual provider distributions that haven’t missed a beat.

Proven Financial Results
Our track record shows consistent savings that strengthen your bottom line:
- Achieved payback on investment within 18 months
- Saved Christ Hospital $60M+ over 8 years on employee health plans
- Distributed savings to providers every year since inception

Measurable Clinical Improvements
Our physician-led approach drives better health outcomes:
- Maintained 80%+ patient engagement rates through physician-led outreach
- Reduced avoidable hospitalizations across Hamilton County
- Improved chronic illness management through targeted physician-patient partnerships

Real Physician Benefits
We keep doctors engaged by respecting their time and expertise:
- Fair compensation for previously unbilled care management hours
- No new IT systems or burdensome documentation required
- Equal distribution model for employed and affiliated physicians
The Proof Is In Our Extensive Expertise

Unmatched Experience
Dr. TJ Redington has shaped population health management at every level, from direct patient care to state-wide programs. He served as Medical Director for Ohio Medicaid, was a Professor of Internal Medicine at the University of Cincinnati, pioneered chronic illness care redesign, and became a nationally recognized clinical transformation expert.

Proven Results
While others talk about potential, we deliver consistent results. Our Clinically Integrated Network consulting work at Christ Hospital shows what we can do: eight years of savings, physician bonuses, and top performance.

Practical Innovation
We bring advanced health strategies down to earth. Our solutions work with your existing systems to deliver real results.
Client Spotlight
The Christ Hospital CIN Success Story: From Vision to $60M in Savings Challenge

Challenge
In 2012, The Christ Hospital needed to prepare for the healthcare industry’s shift toward value-based care while maintaining financial stability and physician engagement.

Solution
Under Dr. TJ Redington’s leadership, the hospital established a CIN focused initially on employee health plan spending. The initiative was physician-led, identifying and engaging high-cost patients while engaging primary care providers. The approach used existing data systems and brought together both employed and affiliated providers under one unified strategy.

Results
The program has delivered documented savings across eight consecutive years of operation, with provider distributions maintained every year since the program began. Quality metrics have shown steady improvement year over year, while the system has maintained exceptional care standards throughout.

“TJ Redington has successfully directed Christ Hospital’s Clinically Integrated Network for 8 years. The consistent financial savings have allowed a physician distribution in each year of operation. The CIN’s durability of cost containment and high performance over this period has been exceptional.”
Justin Chamblee
President
The Coker Group
Maximize Impact with Our
Proven Process

Strategic Assessment
We evaluate your current operations and pinpoint untapped opportunities for immediate cost reduction and long-term value creation.

Physician Engagement
Our physician-led team works directly with your providers to create buy-in through a shared vision of success and clear financial incentives.

Implementation
We activate proven cost-control strategies through your existing systems, targeting high-cost patients and optimizing care delivery for immediate savings – just like we did at Christ Hospital.

Ongoing Optimization
We keep fine-tuning your results, helping you maintain consistent savings while building your ability to succeed in contracts where insurers reward better outcomes and lower costs.
Immediate Benefits, Long-Term Results

Financial Impact
We rapidly deliver measurable results while building sustainable long-term value.
- Typical savings of $20-30 million within the first 24 months
- Return on investment achieved within 18 months
- Sustainable cost reduction year over year

Physician Relations
Our physician-led approach creates equal partnerships that work for everyone.
- Doctors earn yearly bonuses based on cost savings
- Enhanced provider satisfaction and retention
- Equal treatment of employed and affiliated physicians

Operational Excellence
We help you identify and solve your biggest problems.
- Improved management of high-cost patients
- Better patient health outcomes
- Reduced employee turnover
- Better usage of existing resources
Redington Group versus Others
| Others | The Redington Group | |
|---|---|---|
| Core Specialization | Traditional healthcare consulting firms focusing on broader healthcare transformation | Healthcare consulting focused on Clinically Integrated Networks (CINs) |
| Cost Savings Track Record | Varying results without specific documented long-term savings claims | Documented savings of over $70 million in 8 years for a single healthcare system |
| Provider Engagement Model | Standard consulting models often lacking direct physician leadership | Physician-led and physician-run approach with consistent annual provider distributions |
| Implementation Approach | Often begin with broader system-wide changes or ACO implementations | Starts with employee health plans to demonstrate immediate ROI |
| Fee-for-Value Transition | May advocate for immediate full transition to value-based care models | Specialized focus on transitioning from Fee-for-Service using CINs as stepping stones |
| Client Focus | Various healthcare organizations with different transformation goals | Healthcare systems seeking to improve operating margins through employee health plan optimization |

Common Concerns, Real Solutions

“We don’t have the bandwidth for another initiative”
Our strategy requires minimal additional resources and uses your existing IT infrastructure. Most systems see positive ROI within 18 months.

“Our physicians won’t buy in”
Our physician-led method consistently achieves high engagement rates through meaningful financial incentives and improved patient care models.

“We’re not ready for value-based care”
Our program starts with your employee health plan, creating a low-risk environment to develop and refine your value-based capabilities.

“We’ve tried ACOs before with minimal results”
Our CIN model is different—by starting with employee health plans, we create immediate wins while building capabilities. Our track record shows consistent savings and distributions every year for 8 years.

“We’re worried about implementation costs”
We leverage your existing IT systems and data infrastructure, focusing on optimizing what you already have rather than expensive new investments.

“How do we know this will work for our specific system?”
We begin our Clinically Integrated Network consulting with a complete assessment of your current operations and employee health spend, identifying specific opportunities before making any changes. Your path forward is customized to your system’s unique needs.
Life without Redington Group

Beyond Fee-for-Service
Healthcare costs rise while rewarding procedures over outcomes.

Limited Provider Engagement
Providers remain uncompensated for additional office hours and care management.

High Employee Healthcare Costs
Spend continues to increase year after year without effective cost control.

Growing Patient Demands
No systematic way to identify and manage high-cost patients who drive 80% of expenses.

Squeezed Operating Margins
Cost increases outweigh managed contract annual increases.

Missing Value-Based Tools
Unprepared for transition to risk-based contracts.

Provider Turnover Risk
No additional incentives to retain healthcare providers.
Life with Redington Group

Proven Cost Savings
Millions saved over 8 years with consistent year-over-year savings.

Enhanced Provider Satisfaction
Annual distributions to clinicians from savings, creating stronger provider relationships.

Efficient Patient Care
Targeted management of high-cost patients with improved outcomes.

Increased Operating Margins
Immediate benefits to the bottom line through employee health plan optimization.

Value-Based Care Done Right
Strategic pathway from fee-for-service to fee-for-value.

Better Employee Benefits
Concierge level care for employees with lower healthcare costs.

Enhanced Provider Retention
Fair pay and good conditions engage providers fully.
Getting Started with Clinically Integrated Network Consulting is Simple

Step 1
Schedule a consultation with our team
Fill out our quick contact form, and we’ll reach out within 24 hours

Step 2
Receive a customized assessment of your opportunity
Get a detailed analysis of your system’s potential for improvement

Step 3
Review our detailed implementation plan
See exactly how we’ll help you achieve measurable results

Step 4
Begin your journey to improved outcomes
Start your transformation with a proven, step-by-step approach
